Rethinking illegal drug policy in Thailand
In a Q&A, Stanford postdoctoral fellow Darika Saingam explains why Thailand's battle against drugs continues and what is needed to introduce good policy that works to prevent illegal drug trade and supports recovering addicts.
Despite Thailand’s decade-long crackdown on drugs, demand for illegal substances has risen. A green leaf drug known as ‘kratom’ is a symbol of this rise as young people eagerly adopt the drug for entertainment and join an older generation of laborers who chewed it to survive long hours of work in the fields—and are now heavily addicted. Curtailing substance abuse and its consequences takes good public policy and solutions must be area-specific and evidence-based, according to a Stanford postdoctoral fellow.
Darika Saingam, the 2015-16 Developing Asia Health Policy Postdoctoral Fellow, has conducted two cross-sectional surveys and more than 1,000 interviews with drug users, recovered addicts, and local public officials in an effort to better understand the evolution of substance abuse in southern Thailand.
At Stanford, she is preparing two papers that offer policy options suitable for Thailand and other developing countries in Southeast Asia. Saingam spoke with the Shorenstein Asia-Pacific Research Center (APARC) where she will give a public talk on May 17. The interview text below was edited for brevity.
For decades, Thailand has been an epicenter of drugs. Can you describe the extent of the problem today?
According to a 2014 report, 1.2 million people were involved in illegal drug activities across Thailand. The total number of drug cases saw a 41 percent increase from 2013 to 2014. New groups of drug traffickers are mobilizing while existing groups are still active. Drug users who are young become drug dealers as they get older. The number of drug users below 15 years of age has increased dramatically.
According to your research, what drives Thais toward illegal drug use and the trafficking business?
Adults in Thailand use drugs to relieve stress and counteract the effects of work. Adolescents use them for entertainment. Historically, farmers and laborers from rural areas of Thailand would use opium for pain relief. More recently, a consumable tablet known as yaba has become popular along with crystal methamphetamine and marijuana. Young people are increasingly using yaba and kratom.
Thailand is still a developing country, but it is industrializing quickly. Social and cultural norms have been shifting and people want an improved quality of life. A lot of young people are unemployed and lack social support and are therefore more likely to turn to drug trafficking for economic opportunity. The economic recession and political strife in countries bordering Thailand have exacerbated the situation.


Photos (left to right): A man holds up a kratom leaf. / Saingam examines kratom leaves as part of her research to understand illegal cultivation practices.
What is kratom and why is it popular?
For nearly a century, the native people of Thailand have chewed kratom. It is a leaf that grows on trees resembling a coffee plant. Historically, kratom was used to reduce strain following physical labor, to be able to work harder and longer, and to better tolerate heat and sunlight. Kratom is also embedded in Thai culture and given as a spiritual offering in religious ceremonies. My field research in the southern province of Nakhon Si Thammarat has shown that these motivations are still true today.
Within the past seven years, kratom use has skyrocketed and people are using it in increasingly harmful ways. Chewing kratom is not immediately harmful to health, but combining it with other substances is. This is the recent trend. Users have created new ways to consume it such as in a drink known as a ‘4x100.’ It contains boiled kratom leaves, cough syrup and soft drinks. Additional methamphetamines and benzodiazepines are sometimes added to that mixture.
What strategies must be employed to control substance abuse?
The first step is to realize that the patterns of substance abuse are specific to each location therefore solving the problem must also be. Drug usage is also dynamic. Placing hard control measures on one substance often provokes the emergence of another in its place therefore a holistic approach is important.
Thailand should employ multiple strategies toward effective prevention and control of substance abuse. These strategies include examining the problem and creating policies from an economic perspective (supply and demand), an institutional perspective (national and international drug control cooperation), and a social perspective (structural supports for recovered addicts and mobilization of public participation).
What is the Thai government doing to address the drug problem, and what could they be doing better?
Politicians in Thailand must do a better job at representing the people. Government health workers are often gathering information, assessing needs, and reporting findings to politicians, but these needs are not being accurately addressed. An example of this is politicians ordering to cut down kratom trees – a public display that does not get at the root cause of the problem. The reality is that drug users will quickly find substitutes. According to my study, of the regular users that stopped using kratom, more than 50 percent turned to alcohol instead and did so on a daily basis. This is merely a shift from one substance to another.
On the upside, a crop substitution program created under King Bhumibol Adulyadej offers a successful working model. The program works to replace opium poppy farming with cash crop production. It began in 1969 and is cited for helping an estimated 100,000 people convert their drug crop production to sustainable agricultural activities. Crops cultivated can be sold for profit in nearby towns. The program has also introduced a wide variety of crops and discouraged the slash-and-burn technique of clearing land. It is win-win because it stymies drug trade and provides economic opportunity while also being ecologically sound. This type of program should continue to be scaled up.
Can this model be co-opted elsewhere? What lessons from other countries could inform Thailand’s approach?
Yes, the model could plausibly be implemented in other areas in Thailand and in other Southeast Asian nations.
I think a judicial mechanism such as the kind seen in France could benefit the rural areas in Thailand. The French government has established centers across the country that act as branches of the court that try delinquency cases of minor to moderate severity, and also recommend support services for drug users. Members of the magistrate and civil society actors manage center operations thus placing some responsibility back onto the local community.
I believe an opportunity also exists for Thailand to legalize kratom. Legalization would show a respect for the cultural tradition of chewing kratom leaves and allow the government to suggest safer ways of using it. Bolivia has created a successful model of this through its legalization of coca leaves. Coca in its distilled form is cocaine, but left as a leaf, it is not a narcotic. Indigenous peoples are allowed to chew coca leaves. The government policy is being credited for a decrease in cocaine production as well.






 Hangzhou, Zhejiang Province, China. Photo credit: Wikimedia Commons
Hangzhou, Zhejiang Province, China. Photo credit: Wikimedia Commons
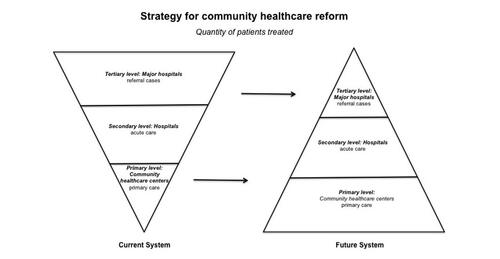 Courtesy: Feng Lin
Courtesy: Feng Lin





